Corneal disease can range from the simple to the complex. Much of it can be handled by your doctor of optometry. In the event that you have a complex problem requiring advanced medical or surgical care Dr. William Bond is ready to serve you.
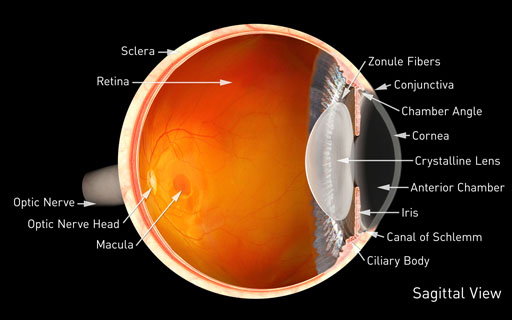
The cornea is the clear front window of the eye. It transmits light to the interior of the eye allowing us to see clearly. Corneal diseases can cause clouding and distortion of vision, and eventually blindness. There are many types of corneal disease. Infections related to contact lenses, abrasions from trauma, and inflammation are common. Other conditions include keratoconus, Fuchs' endothelial dystrophy, and pterygia among many others.
Symptoms of Corneal Disease:
- Infections or inflammation along with corneal abrasions will often cause a feeling that something is in the eye, with sensitivity to light and a foreign body sensation.
- Corneal ulcers and infiltrates can be caused by bacteria in and around the eye, or by the herpes virus that lives in most of us and can travel to the nerve endings of the eye and become an active infection of the cornea.
- Contact lenses, even when fit properly, can cause a shortage of oxygen to the cornea, essential for proper functioning and clarity of this delicate structure. If your contact lens hygiene is less than optimal, or you don’t replace lenses as frequently as necessary, the cornea will eventually “protest” and cause symptoms such as redness, irritation, and blurring of vision.
- Dry Eye syndrome is common and can cause significant damage to the cornea. Some people don’t produce enough tears, and others have eyes that don’t close fully to protect the cornea and keep it moist at night. Others have chronic lid infections, a common condition known as blepharitis, that causes an unstable tear film and can aggravate dry eye along with causing inflammation of the corneal surface.
- With keratoconus, as the cornea protrudes or steepens, vision becomes increasingly blurred and contact lens wear, which is often an early treatment for the disease, becomes difficult. The contact lens may not stay on the eye due to the irregular shape of the cornea.
- A person with Fuchs' endothelial dystrophy or bullous keratopathy may first notice glare with lights at night or in bright sunlight. As these conditions progress, vision may be foggy or blurry in the morning and clear up as the day progresses. As the diseases further progress, vision will stay blurrier later into the day and eventually may not clear at all.
- Occasionally people develop a fleshy growth on the white part of the eye that then extends onto the cornea, leading to redness, blurred vision, and an undesirable cosmetic appearance. This growth is called a Pterygium and can be removed surgically.
Keratoconus is a weakening and thinning of the central cornea. The cornea develops a cone-shaped deformity. Progression can be rapid, gradual or intermittent. Keratoconus usually occurs in both eyes, but can occur in only one eye. This may start as ASTIGMATISM, which many people have a small amount of, but in higher irregular degrees, it can be difficult to correct with glasses or even contact lenses.
Fuchs' endothelial dystrophy is a hereditary abnormality of the inner cell layer of the cornea called the endothelium. The purpose of this layer is to pump fluids out of the cornea, keeping it thin and crystal clear. When the endothelium is not healthy, fluids are not pumped out and the cornea develops swelling, causing it to become cloudy and decrease vision. This can lead to Bullous keratopathy, a condition in which the cornea becomes permanently swollen. This occurs because the inner layer of the cornea, the endothelium, has been damaged and is no longer pumping fluid out of the tissue.
Causes of Corneal Disease:
- Infection: Bacterial, fungal and viral infections are common causes of corneal damage.
- The cause of keratoconus in most patients is unknown.
- Age: Aging processes can affect the clarity and health of the cornea
- Cataract and intraocular lens implant surgery: Bullous keratopathy occurs in a very small percentage of patients following these procedures.
- Heredity
- Contact lenses
- Eye trauma
- Certain systemic diseases
Diagnosing Corneal Disease:
Your eye doctor can check for corneal disease and trauma by examining your eyes with magnifying instruments. Using a slit lamp and advanced diagnostic technology such as corneal topography, your doctor can detect signs of corneal infection, inflammation, scarring, and other problems associated with the front structure of the eye. A special dye may be used to determine the extent of the damage.

A slit lamp can detect corneal disease at an early stage
Treatment for Corneal Disease:
As with any serious eye infection, corneal disease should be treated immediately. There are antibiotics and steroids that can be used topically, and occasionally by mouth, to treat the myriad of conditions that can affect the cornea. It is important NOT to use a friend’s eye drops or Visine like drops without consulting your ophthalmologist.
A corneal transplant is sometimes necessary to restore vision when the cornea becomes clouded, but newer advances like Endothelial Keratoplasty or DSAEK may also be employed in certain cases to help restore vision.